Do you leak a little urine when you cough laugh or sneeze?
Half of the women over the age of 50 with experience some symptoms of pelvic organ prolapse, with 1 in 10 women by the age of 80 undergoing surgery. Worryingly, about a third of these women will need more than one operation. A mild prolapse often causes no symptoms and treatment is not always necessary. However, you should see your doctor if you think you may have a prolapse Please don’t be embarrassed, suffer on silence ore rely on incontinence pads.
What causes a prolapse
The organs within a woman’s pelvis (uterus, bladder and rectum) are held in place by ligaments and muscles known as the pelvic floor. If these support structures become weak, the pelvic organs can slip or bulge (prolapse) from their natural position into the vagina. Sometimes a prolapse may be large enough to protrude outside the vagina.
Symptoms
Prolapse can affect the quality of life by causing symptoms such as discomfort or a feeling of heaviness. It can cause bladder and bowel problems, such as frequency, urgency or leakage . A prolapse can also affect sexual activity.
Types of pelvic organ prolapse
There are several different types of prolapse, which are graded in severity; first, second or third-degree prolapse.
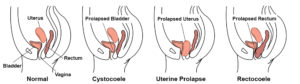
- Uterine prolapse: the uterus and cervix slip down into the vaginal canal .These all involve a weakening of the supporting structures resulting in a dropping or descend and pressing into the wall of the vagina.
- Cystocele: The wall between the bladder and vagina – resulting in part of the bladder and the vaginal wall
- Urethrocele: The urethra (tube leading from the bladder to the outside of the body) is affected. Note usually occurs with a cystocele.
- Rectocele: The wall between the vagina and rectum resulting in the rectum
- Enterocele: Similar to a rectocele, but instead involves the area between the uterus and the rectum (Pouch of Douglas)
- Vaginal vault prolapse: A vaginal vault prolapse occurs when the top of the vagina descends in women who have had a hysterectomy.
What can you do
- Avoiding getting constipated or straining to open your bowels
- Stopping smoking,
- Moderate exercise, running may not be advisable
- Avoid activities that may make your prolapse worse such as heavy lifting
- Treatment options
Mild cases, pelvic floor exercises are the first line (see post next post for details)
Specialised women’s health physiotherapy
Using prescribed pessaries
Corrective surgery. Not everyone with prolapse needs surgery but you may want to consider surgery if other options have not adequately helped. Surgery for prolapse aims to support the pelvic organs and to help ease your symptoms. It cannot always cure the problem completely.
Still confused? Sign up for my Pelvic floor explained workshop
Please note: This is for guidance only, it should not be regarded as a substitute for medical advice, diagnosis or treatment given in person by an appropriately trained health professional







