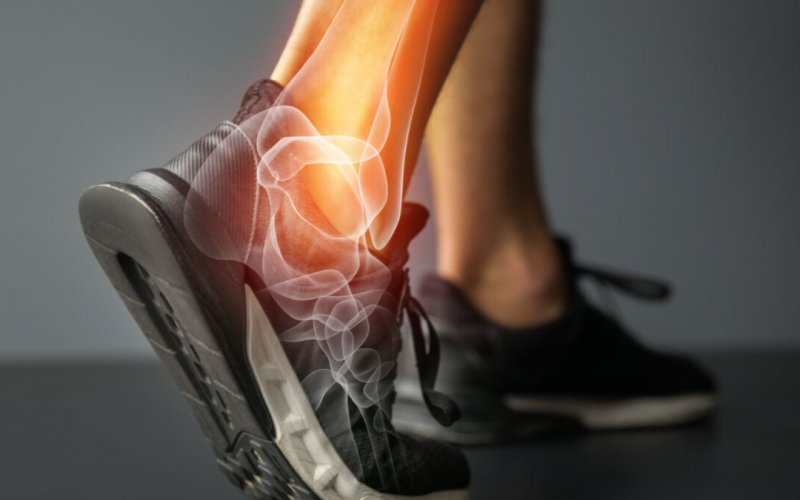
Achilles tendon pain is sporting complaint often seen in runners and tennis players. People report stiffness or pain in the back of the heel. Achilles tendonitis is an overuse injury due to the repetitive action and so may occur in other repetitive activities.
There are many different terms uses to describe a tendon injury.Most health professionals now use Achilles Tendinopathy: which includes both inflammation and micro-tears. However, some people may still use the following terms out of habit
- Tendonitis: ‘itis’ means inflammation, but research informed use that inflammation is rarely the cause of tendon pain.
- Tendinosis: tiny tears in the tissue in and surrounding the tendon usually caused by overuse.
What is it?
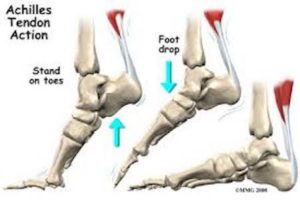
The Achilles is the tendon that attaches the calf muscles to the calcaneus (heel bone). The two calf muscles form it, the gastrocnemius and soleus, which join to insert on to the heel bone. More, the Achilles tendon is a little shock absorbing spring; it has to tolerate the highest loads in the body up to 10 times our body weight during running, jumping and skipping.
What Causes Achilles pain
Most tendon injuries are the result of gradual wear and tear to the tendon from overuse or ageing. There are some other, other potential causes of Achilles pain which need careful screening before starting treatment
- Posterior impingement of the ankle: causes pain in the same area but Forced plantar flexion (pointing) of the ankle will be painful.
- Partial tear of the Achilles tendon: this is easily missed even by experienced practitioners and requires very different treatment.
- Nerve pain that mimics as tendon pain.
Classic features of Achilles tendinopathy
- Usually a gradual onset of morning stiffness which may resolve within 5-10 minutes
- Stiffness when walking especially after prolonged sitting
- Stiffness is often worse the days after running
- The pain/stiffness will typically improve after the warm-up phase of sport, after first 5-10 minutes of a run.
- Pain and stiffness are often worse at night or-or first thing in the morning.
- The area may be tender, red, warm, or swollen if there is inflammation.
- A crunchy sound or feeling when you use the tendon.
- There may be a loss of strength in the affected area
- There may be a noticeable lump painful within the tendon.
As symptom are variable and often not constant, people often delay seeking advice, as they can initially run through the pain. However, studies have demonstrated that the earlier you seek treatment, the more likely are to manage with making adjustments rather than stopping activities altogether.
Risk factors Achilles tendinopathy
 More men are affected than women
More men are affected than women- Aged 30 – 50. S
- Over-training or “too much too soon.”
- Poorly supportive footwear
- Over-pronated (flat )feet
- Change in training surface e.g. grass to pavement
- High foot arch with tight Achilles tendon
- Tight hamstring and calf muscles
- Toe walking (or regularly wearing high heels)
- Running up or down hills.
- Asymmetry of the lower limb
- Poor dynamic control of a movement
- Poor eccentric strength
How is Achilles Tendonitis Diagnosed?
Usually by a physical therapist or osteopath, with a combination of the history, symptoms behaviour and clinical tests. In addition, a sports doctor can usually confirm the diagnosis of Achilles tendonitis with an ultrasound scan
Management
As previously mentioned its a common problem seen in runners and other high impact sports people including weekend warriors. Unfortunately, it is prone to recurrence if people resume exercise too quickly, especially if they didn’t adhere to or complete a thorough rehabilitation programme. Tendons have a different level of blood supply and function, which does alter the rehabilitation process, sadly it takes longer.
In the early phase you may be unable to walk without a limp, so your Achilles tendon needs some active rest from weight-bearing. Use crutches, a wedged Achilles walking boot or heel wedges to relieve some of the pressure on the Achilles tendon temporarily. Your practitioner (osteopath, physiotherapist or sports doctor) will advise you on what they feel is best for you.
Achilles Tendinopathy first aid
As with most soft tissue injuries, the initial treatment plan is
- RICE – Rest, Ice, Compression and Elevation.Click here for how to information
Principles of treatment
- Regain full range of motion with manual therapy
- Strength training and correcting training errors
- Restore eccentric muscle strength
- Restore concentric muscle strength
- Normalise foot biomechanics
- Restore high speed, power, proprioception & agility
- Return to sport
Treatment
There is no precise time span for when to progress from each stage to the next. For example, Achilles recovery will be affected by many factors, including the severity of the tendon injury, patient compliance with treatment and home exercise. In most cases, your practitioners will seamlessly progress between the rehabilitation phases as your clinical assessment and function improve.
What Results Should You Expect?
There may be a need to stop running initially, but there is now general agreement amongst manual and physical therapist that off-loading the tendon for too long is unhelpful. Importantly, with careful assessment some running may be undertaken if symptoms allow and is necessary for a successful recovery. Coupled with assessing morning symptoms (stiffness and pain) this can be a good indication of how the tendon is coping. Recovery times do vary, three to six months is the usual but anything up to nine months is not uncommon.
Can Your Achilles Tendon Rupture?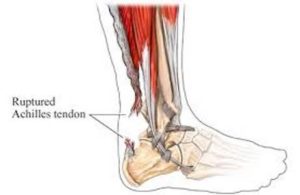
The worst case scenario is a total Achilles tendon rupture; these usually require surgical repair, a plaster cast or a walking boot for at least six weeks.
Followed by a six – 12 months period of rehabilitation.
Final thoughts, if have Achilles pain, soreness or stiffness seek early advice from a sports doctor, osteopath or physiotherapist to do all you can to avoid a possible Achilles tendon rupture occurring in the first place.Achilles tendon pain
Please note: This is for guidance only, it should not be regarded as a substitute for medical advice, diagnosis or treatment given in person by an appropriately trained health professional.